Contents
Overview
As a team, we decided to devolve considerable attention to human practices because we wanted to analyse in depth the factors that could have had an impact on our project from a multi-dimensional perspective including ethical, political, and economic factors. In particular we wanted to examine how these elements could have made a difference on the success of our project, therefore we decided to incorporate all of the factors we have found to be relevant to our project into the development of the project itself. Some specific factors regarding public preferences, such as reaction times of the biosensor were incorporated into the project after having collected feedback through public engagement activities. Such modifications were implemented throughout the creation of our biosensor. Information gathered from major stakeholders (see below) influenced the design of our biosensor hardware as we worked to scale down the costs and improve the effiency of our first-generation models while ensuring safery concerns that were brought up were adequately met in our final version. In general, we considered integrated human practices as a continual process that took into account public interest and preferences aimed to integrate social science into our project from the very beginning. We applied this concept of interdependence between human practices, therefore social science, and the project itself, classified as synthetic biology, so that the two variables could be interdependent throughout the entire project instead of classifying them as two separate entities. All of the following considerations regarding the political, economic, social, and ethical sphere have been implemented into our project in order to provide an exhaustive and potentially realistic expectation of how our research project could be actualised in the real world.
PEST Analysis
As part of our gold medal requirements for human practices, we have decided to use an analytical framework largely used within social sciences, the PEST analysis. PEST (political, economic, social and technological) describes a framework of macro-environmental factors used in the environmental scanning component of social sciences. We have decided to use a PEST analysis for our iGEM project to examine in a structured way those macro-environmental factors that will have an impact on the implementation of our project. Even though PEST is usually used for business management and organisational purposes, we recognised that such an approach would have represented a useful tool for integration of social science into our synthetic biology project. As human practices tend to emphasise the importance of how factors outside of the laboratory should affect our work, and how our work affects the world outside, a PEST analysis has helped us determine the weight that each one of those factors will have on the success of our project. The outcomes of this analysis also influenced the different design iterations of our biosensor device, especially as pertaining to EU-standards.
Political
In terms of political factors, we researched, then incorporated public policy as well as legal considerations to have a comprehensive political framework for our project. In this regard, Dr Chris French from the Arsenic Biosensor Collaboration, has helped us greatly to understand the challenges that political and legal factors could pose to our research project. This year we have considered legislation regarding both the use of GMO biosensors within the European Union, as well as regulations on food hygiene standards and general food safety law. In addition, we have devoted interest to recent political changes that might affect our project; specifically, the potential implications that Brexit will have on future UK legislation. In terms of GMO legislation, we have found out that the central issue is the use of live genetically modified organisms outside a contained and properly registered laboratory. This is covered in the EU by 2009/41/EC for contained use and 2001/18/EC for deliberate release into the environment, or in the UK, the Genetically Modified Organisms (Contained Use) Regulations 2014. In terms of food safety law and food hygiene legislation, we have considered several policies that the UK has been adopting in order to ensure that farming, food safety management procedures, and food hygiene regulations are being kept at high standards. Some of these policies include the Regulation (EC) 178/2002, which set out the general principles and requirements of food law in the EU; and EU Regulation 882/2004 on official controls for feed and food law (and animal health and animal welfare) sets out the approach that competent authorities of member states must adopt for official controls. Since most of the legislation we have considered is EU-derived, we believed it would be useful to analyse the potential impacts that an upcoming exit of the UK from the EU would cause to the future of such policies. For this reason, we have dedicated particular attention to the recent political turmoil that has been characterised by uncertainty on the future of national legislation. A detailed policy brief can be found here.
Economic
In terms of economic impacts of our project, our main priority is to create a biosensor that will be economically advantageous compared to current costs that laboratories face when testing chicken for Campylobacter. When researching current data on economic costs associated with this, we asked Scotland's Rural College about current procedures used for testing chicken for Campylobacter. At present the procedure includes swabbing the birds, sending the swab to the lab and get the results up to a week later. We were told that an instant result would have been most helpful. In order to establish the economic costs associated with such a procedure, we analysed figures that determined the current costs, technologists’ time, and time to a positive and negative result using conventional culture methods. The figures were provided by the Department of Pathology, University of Texas Southwestern Medical Center [1], that recorded the costs per stool culture for media and reagents. According to the statistics, average costs for media and reagents for cultures were as follows: No potential pathogens, $5.74 (£4.28) (n=74); negative cultures with additional workup, $7.27 (£5.43) (n=127); and positive cultures, $9.33 (£6.96) (n=5). Shigella sonnei, Campylobacter species and Salmonella species were the bacterial pathogens that were recovered in the 5 positive cultures. To evaluate the technologists’ time, 5 different technologists recorded the time that they spent on stool workups. The average technologist time required to complete a single final culture was approximately 8 minutes (range of 1-15 minutes). Using an average cost of $27 (£20.16) per hour for technologists’ labour and benefits and 8 minutes of time per culture, the labour cost per culture was $3.60 (£2.69). Including media, reagents and labour, the average cost to detect a single positive culture was $427 (£318.76). While negative cultures with no potential pathogens were reported at 48 hours, positive cultures required 72 to 96 hours to finalise. Our aim is to reduce the economic impact that comes with swabbing and using laboratory facilities, by providing a more affordable alternative that saves users both time and money. On a macro-scale, being the UK economy enormously affected by Campylobacter related infections, our biosensor will serve as a tool to benefit macro economic issues.
Social
Our targeted stakeholders can be divided into three categories; farms, industrial kitchens, and private customers at home. Therefore, the biosensor was designed to be able to detect Campylobacter in a way relevant to all stages of the poultry process, from farm to fridge, even though it will serve the same purpose. The social factor was particularly important to us as human health is the main reason behind our research project. We wanted to find a quick and easy solution for an issue that negatively affects us, since Campylobacter related infections represent an enormous issue for human health in the UK as well as in the rest of the world, but they are so easily preventable that the amount of infections could ideally drop to zero with education and prevention.
Technological
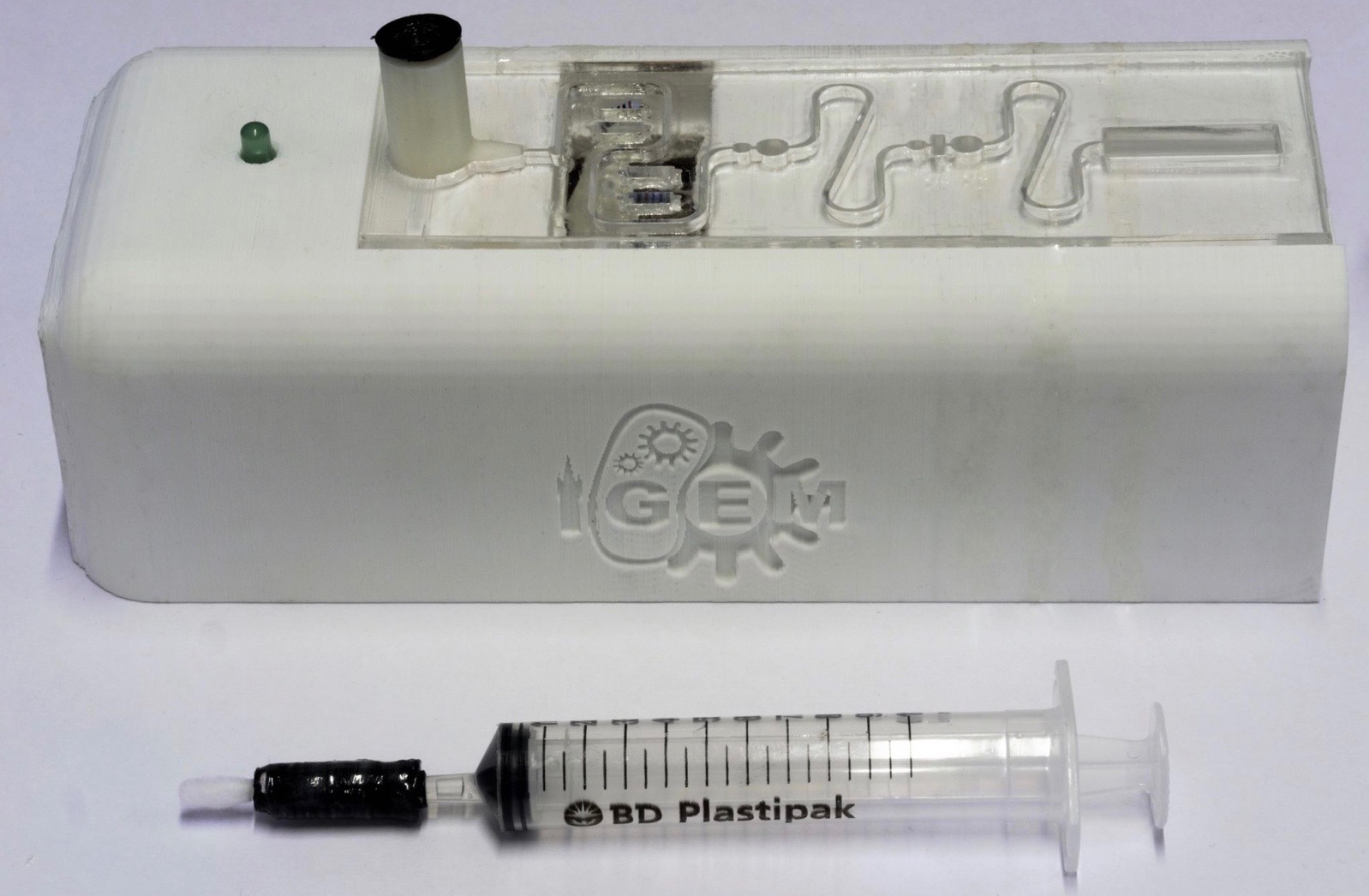
We will make a functioning genetically engineered biosensor. Our fluidic biosensor device consists of 3 elements:
- Swab attached to a syringe containing 1% acetic acid
- Fluidic channel processing plate for preparing the sample for detection
- Heating Element driven by a separate electronic circuit
An area of interest (e.g. a carcass, or a work surface) is swabbed; the syringe-swab is then inserted into the input section of the device’s processing plate. The syringe is the depressed slowly, washing the sample from the swab with 1% acetic acid and passing it through the device. The device prepares the sample for detection through a series of stages which will release the sugar xylulose from the capsule of any Campylobacter bacteria present. These stages include:
- Heating the 1% acid and sample mixture to 100 Degrees Celsius. This liberates xylulose from the extracellular capsule of Campylobacter)
- Neutralising the acid using a Tris-Acetate buffer (making the solution innocuous to the biosensor detection organism, either E. coli or Bacillus subtilis)
- Demonstrating the pH neutralisation of the sample by using litmus paper
- Mixing with glucose growth media (ensuring the biosensory strain does not metabolise the xylulose)
After the stages mentioned above, the sample is ready to be delivered to the detection chamber. Here, depending on the final design, a strip of filter paper has either been pre-prepared with a hydrogel coating that contained our genetically modified E. coli , or there a sample of dried biosensing Bacillus subtilis spores. The liquid sample enters the chamber to diffuse into the cells, which should then respond to the presence of xylulose (or any other potential Campylobacter specific molecular markers designed into the genetic construct) by expressing a coloured protein, such as RFP (red fluorescent protein). The detection chamber, along with the rest of the device, is transparent, allowing the user to observe any colour changes should xylulose be present in the sample.
Acting on Campylobacter Together Campaign (FSA)
As part of our integrated human practices, we decided to reach out to regulators in order to have a better idea of the future of the legislation regulating hygiene standards in the UK industry. We wanted to know what exactly are the protocols to follow to make sure campylobacter levels are minimised and the criteria that regulate hygiene standards. These regulators in the UK are represented by the Food Standards Agency. We were lucky enough to receive a response from the FSA that accepted to speak to us and answer our questions. The FSA has been promoting in recent years a campaign that aims to educate the public on what campylobacter is and how to prevent food poisoning, called “Acting on Campylobacter Together”. From their figures, an extensive portion of the public was not aware of what campylobacter is, or how to minimise the risk of foodborne related infections; however, almost 30% of people reported concern about food poisoning [2]. In the following section, we report our conversation between the FSA’s Foodborne Disease Control policy group, and our iGEM team. In addition, we have provided some important selected figures that the FSA has kindly shared with us [3].
What is the protocol in the UK if there is an outbreak of a poultry bacterium?
Our first question regarded any potential protocol that the industry needs to follow if there is an outbreak of a poultry bacterium. We found out that there isn’t any protocol at the present time that regulates this. At the moment there is a lack of regulation governing the levels of Campylobacter in the UK. There is a process for food hygiene criteria but there is a lack of food safety criteria. Slaughterhouses must assess their hygiene standards and make adjustments accordingly; however, they can choose not to disclose their hygiene scores.
According to the FSA, there will be an initial EU legislation enforced in January 2018 regulating better hygiene criteria in the food industry, and this legislation will be implemented despite the Brexit negotiations.
What is the legislation regulating Campylobacter levels in food outlets?
We also asked the FSA whether there is legislation for food outlets in terms of Campylobacter levels; and once again there is a gap in legislation regarding Campylobacter. Hygienic preparation standards exist and outlets have a responsibility to produce safe food. Due to these there is a target of 103 colonies per gram, in no more than 10% of tested products. The EU has food hygiene laws and the overarching message is that food outlets should produce safe food; however, the way this is regulated is still extremely unstable. In England and Scotland, it is voluntary to post hygiene scores at restaurants.
Accordingly, there are two types of restaurants:
- restaurants that voluntarily disclose their hygiene scores on their doors and
- restaurants that do not disclose scores on their doors.
However, the FSA’s dataset does not track voluntary disclosure status. We have also found that no academic study has investigated the economic incentives behind this voluntary (non-)disclosure; therefore, there is also a gap in academic literature.
What is the position of the UK on chlorine-washed chicken?
We asked regulators about their position of chlorine washed chicken. We found this discussion extremely interesting as there seems to be profound disagreement between the EU and US position on the topic. According to the FSA, the UK’s position is that they do not perceive chlorine-washed chicken as a problem or cause of trouble; the EU however does not allow chlorine washes of poultry products. Whether or not the UK laws will change post Brexit is an issue that will be decided during subsequent trade negotiations. The FSA has performed public focus groups that appear to be reluctant to accept chlorine-washed poultry, as does the supermarket industry for fear of lost sales. In addition, the British Poultry Council has also come out against chlorine washed chicken. To find out more about the debate on chlorine-washed chicken please have a look at the page.
What are the practices used to reduce Campylobacter levels?
We analysed figures that stated that in 2016, 65% of chicken carcasses in the UK were contaminated with Campylobacterr. In 2017, figures were sitting at around 50%. Therefore, we enquired about the remaining 35-50% which weren’t contaminated, and asked for further clarification on the practices used by the industry. The FSA has been promoting a national campaign that emphasises the importance of raising awareness on the dangers caused by Campylobacter; the campaign has worked with industry to help reduce the bacterial load on chicken carcasses in the UK. In the slaughterhouse there are two practices they have encouraged, and they mainly break down into hot and cold interventions. In the hot intervention, the carcasses are scalded at 80oC for a few seconds to help reduce the bacterial load on the carcass. In the cold intervention, the carcasses are sprayed with liquid nitrogen or super cooled air to help reduce bacterial load. In farms it is becoming more common to segregate certain sheds to help reduce the potential for cross contamination. It is useful to note that these interventions are not always 100% effective in every factory. The practice of the techniques can affect the outcome.
We asked regulators whether they had seen an increase in the utilisation of hot and cold interventions, used in order to prevent Campylobacter from developing. From their figures, it seems that 85% of the industry producers of chicken in the UK have taken up these interventions and the FSA is hoping to get the rest to do that as well, therefore they hope to see the continued use of such interventions in order to further reduce the levels of Campylobacter.
Figures and statistics
As reported by the FSA, consumers do not perceive food poisoning to be a high risk in relation to home-prepared food; and if they do encounter it, they expect it to have limited consequences. The public are confident they can manage the risk from food poisoning when preparing the food themselves. Consumers voiced greater concern about 1) the long term impacts of poor diet and the use of chemicals and additive in food, and 2) what happens outside the home, both in terms of restaurant hygiene and the safety of food production processes.
Consumers are generally content with the current balance of responsibility between consumers/Government and industry. Overall, they are positive about the measures that Government takes to protect them from the risk of food harm. There is however a belief that the Government should educate consumers so they know what the recommended behaviours are – even if they may not act on this information. They also maintained that Government has a responsibility to monitor industry to ensure that standards are maintained and/or improved. There was limited support for industry interventions to reduce food poisoning where this impacted on cost or choice for consumers.
The figures provided by the FSA suggest that 29% of people reported concern about food poisoning. The top food safety issues of concern were: food hygiene when eating out (36%), chemicals from the environment such as lead in food (30%), food poisoning (29%), and food additives (29%).
Conclusion
Food preparation and storage are highly habitual and ingrained and therefore the public tend to rely on their ‘instincts’ about the right thing to do. It may be that household food preparation behaviours will only change after a slow road to social norming via saturation methods for harder to sell messages. Directly challenging strongly held beliefs and habitual practices around food in the home undermines the link between ‘home’, safety and personal efficacy in a way that people often find unacceptable. However, education from the FSA and government with campaigns such as “Acting on Campylobacter Together” has been proved to be helpful to as it has successfully alerted people to hidden dangers in their homes without undermining their sense of personal efficacy or more general safety.
Chlorine-washed chicken
In the context of our human practices, we have decided to devolve some attention to the issue of chlorine washed chicken, which has been a cause of tension between US-EU trade negotiators. The issue has been particularly relevant in recent months because of political changes due to the Brexit referendum. Since, as mentioned in our policy brief, on the 23rd June 2016, the UK has voted to leave the European Union through a national referendum, an extensive amount of trade deals will have to be reconsidered; these include the import of chlorine washed chicken from the US[4]. This is because the EU has banned the import of chicken disinfected with chemical rinses for two decades. Liberalising US poultry imports is expected to be a key feature of US-UK trade talks[5]. To shed light on the issue, we have researched several different sources, so we could have a better understanding on what the different positions are on the topic.
What is chlorine-washed chicken?
In the United States, farms can dip or wash chicken carcasses in water containing chlorine dioxide in order to kill potentially harmful organisms such as E. coli, Campylobacter and Salmonella on the surface of the meat. This happens after animals have been slaughtered and before the meat is packaged. The process is known as pathogen reduction treatment (PRT) in the industry. Other chemicals are also used instead of chlorine dioxide with the most common being acidified sodium chlorite, trisodium phosphate and peroxyacids. Meat besides poultry can also be treated. The EU does not allow producers to wash meat with any substance other than water unless the substance is explicitly approved by the European Commission (EC Regulation 853/2004). Advocates of this approach say that it leads to higher standards of hygiene and animal welfare because farmers must take care at each stage of the process rather than relying on a chemical bath to kill any harmful pathogens after animals are slaughtered.
Is chlorine-washed chicken safe to eat?
The EU has set a maximum residue level of 0.01 mg of chlorate per kg of food. It is not clear how much chlorate is present, on average, in chicken that has been washed with chlorine. The European Food Safety Authority said in 2015 that chlorate is a potential health concern for children but the total intake in current European diets was not enough to cause concern. In a 2005 study, the EFSA found that treating poultry carcasses with the four most-commonly used antimicrobial substances “would be of no safety concern”. It also said that spraying the carcasses rather than dipping or immersing them, as is done in some US farms, would limit the amount of exposure to chemical residues. In a recent article published by Peter Spence, Americans safely eat upwards of 156 million such chickens each week, and adults would need to eat 5% of their bodyweight in chlorinated chicken each day to be at risk of ill health from poultry alone. However, in 2008, the Council of Europe rejected a European Commission proposal to allow the use of antimicrobial chicken rinses containing chlorine, which it said can, “lead to the formation of chloroorganic compounds, several of which are persistent, bioaccumulable or carcinogenic”. In other words, the compounds can cause cancer, are hard to get rid of and have a tendency to build up over time when repeatedly absorbed by living organisms. The Council of Europe did not say anything about how much of the substance someone would have to consume to increase the risk of cancer.
Is washing chicken with chlorine more effective than EU methods?
In 2014, an investigation by the respected independent US non-profit organisation, Consumer Reports, found that 97 per cent of 300 chicken breasts it tested from across America contained harmful bacteria including Salmonella, campylobacter and E.Coli. A 2013 study by the Centers for Disease Prevention and Control - the US federal health protection agency - analysed outbreaks of foodborne illnesses between 1998 and 2008 and found that “more deaths were attributable to poultry than any other commodity”. More than half of the samples in the Consumer Reports study contained faecal contaminants and a similar amount harboured at least one bacterium that was resistant to three or more commonly prescribed antibiotics. A 2016 study by the UK’s Food Standards Agency found comparable levels of contamination in this country - half of chicken samples taken from retailers were infected with multi antibiotic-resistant campylobacter. The latest figures from the FSA show that human cases of campylobacter confirmed by lab tests in the UK decreased 17 per cent in 2016. A 2015 WHO study found that rates of campylobacter infection were similar in the EU and North America. However, it also revealed that infection rates for Salmonella typhi and Salmonella paratyphi were, respectively, four times and five times higher in North America than in Europe. The report does not detail exactly why this difference exists.
What are the benefits of chlorine-washed meat?
Using US government data from 2015, the Adam Smith Institute’s research calculates that US consumers pay 21 per cent less for a kilogramme of chicken than their counterparts in the UK. The think tank therefore advocates negotiating a trade deal that would allow for imports of chlorine-treated meat. The ASI report does not provide evidence demonstrating a causal link between chlorine washing and cheaper poultry prices in supermarkets. Other factors could also be at play. The ASI report also states that the US poultry industry is “far more efficient than that of its European counterparts, making it well-placed to drive down the cost of chicken meat in a post-Brexit UK”.
Conclusion
In conclusion, chlorine-washed chickens are symbolic of much wider concerns around animal welfare and environmental standards that could become a crucial negotiating point in any post-Brexit trade deal between the US and the UK. That trade deal itself is seen as of vital importance to the UK’s future outside the EU; however, as reported by the FSA, a good proportion of the UK appears to be reluctant signing on to this decision, as does industry for fear of lost sales. Proponents, especially in the US, sustain that US methods produce fresh chicken at 79% of the price of equivalent birds on British supermarket shelves, as well as arguing that chlorine-washed chicken is safe to eat. Therefore, British trade negotiators should be authorised to permit the import of chemically disinfected poultry from the US in return for a rapid free trade agreement.
The prospect of chlorine-washed chicken flooding into the UK as the price of a post-Brexit trade deal with the US has garnered a great deal of attention in recent months. At present, it is hard to establish whether the UK will renegotiate this regulation, or comply with the previous EU legislation. However, proponents and opponents alike will have to bear in mind that liberalising US poultry imports is expected to be a key feature of US-UK trade talks.
References
- ↑ Beal, S.G, Mes n, M, Ciurca, J, Smith, G, and Gande, R.M. (2013). Evaluation of costs, technologists time and turn-around times for conventional stool cultures. Department of Pathology, University of Texas Southwestern Medical Center, Dallas, Texas.
- ↑ FSA. (2017). Concern about food poisoning. FSA Public Attitudes Tracker.
- ↑ FSA. (2014). TNS-BMRB Citizens’ Forum Research with consumers. FSA: Balance of Risks & Responsibilities.
- ↑ Chapman, B. (2017). Is chlorinated chicken bad for our health and the environment?. Available: http://www.independent.co.uk/news/business/news/is-chlorinated-chicken-bad-for-our-health-and-the-environment-a7860866.html#explainer-question-0. The Independent. Last accessed 19th Aug 2017.
- ↑ Spence, P. (2017). Chlorine washed chicken. Why we shouldn't give a cluck. Briefing Paper.